One of the topics for Tube Feeding Awareness Week is how we got here.
If you have read my blog at all in the last couple of months you probably know a bit about our journey thus far. If you are new to this blog try THIS and THIS post or the CdLS page for a description of Kaylee's condition and how we got where we are today. But I will start at the start.
When Kaylee was born I thought "Wow she is tiny. Those are some funky little hairy patches on her thighs I wonder what that means. She is beautiful. How am I going to get this tiny baby to latch and feed? How am I going to keep her warm?"
I am a long term breast feeder I guess, having fed 5 kids previous to Kaylee's birth. In fact, for the first half of my pregnancy with her I was still feeding Kaylee's older brother. Feeding my babies has always been one of the most pleasurable aspects of mothering a tiny baby for me. I treasured those moments when I would be forced to slow down and savour their tiny perfection as they guzzled greedily at my breast. For a couple of them, it required work and patience and time to get things working properly, but we always managed it and while I knew it would be a challenge with the tiny infant I had in my arms it didn't occur to me that we wouldn't have a "normal" feeding relationship - I just figured it would take some work. After some rather horrid afterpains I was curled up in bed with a tiny bundle of baby carefully expressing clostrum into her mouth. She lapped at it and opened her mouth but showed no signs of really wanting to attach. After a while we trundled accross to the hospital where I thought they would tell me what kind of syndrome she had and I would take her home to figure out the feeding thing....little did I know.
The next weeks - perhaps months - was a complete blur of hospitals, transports, tubes, wires and a million other interventions and experiences which I do not really care to relive. I know her feeding tube was placed sometime in there - perhaps during her first PICU stay the day after we flew in to Melbourne? That would seem to make sense. I expressed with dogged determination. I remember the first time I managed to express a decent amount of milk. It was the middle of the night and I was reading a message from my oldest daughter which read "Compared to my love for you the sky is like a dot". I carefully screwed the lid on my milk and RAN to Kaylee and cried out to her "Look baby, I made you milk!!" and he nurse very carefully started it going down her feeding tube and into her little tummy. And thus began my love-hate relationship with feeding tubes. As I said a few days ago to another tubie mama - feeding tubes, love that they keep my kid alive, hate every other dang thing about them.
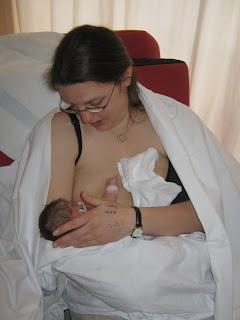
Kaylee was a few days old when we made it up to the cardio ward. It had been a rough few days for both of us but she was finally stable. With the help of Sue, one of the lactation consultants, I put Kaylee to the breast but I have to admit my expectations were very low. I was completely blown away when she actually tried to feed!
It was a balancing act to put her to the breast to try and feed without exhausting her. A combination of a cleft palate, heart condition, poor suck and swallow coordination and poor muscle tone and control all due to her syndrome made feeding very difficult. Because she had the feeding tube, she was able to stay hydrated and well fed which gave her the best chance of learning how to feed for herself. Without the feeding tube, Kaylee would not have survived her first week. We did try her with a special bottle designed for children with special needs but she only got a few mls more than she did at the breast (8ml as opposed to 3 ml, and the bottle tended to try and drown her a bit which wasn't good) so I opted to keep trying at the breast instead because of all the other benefits of direct breast feeding and I had the option to do that because all her milk was getting into her anyway through her tube.
As I researched more and more about Cornelia de Lange Syndrome I learned that reflux was a major life long issue for most people with the syndrome and I became very proactive in asking for her reflux to be assessed and managed with this in mind. Because of the excellent care she received we had little trouble with reflux until after Kaylee's first cardio surgery. Unfortunately after her shunt was placed Kaylee needed to go on a medication which interacted with her reflux medication. She was still on a different medication but it was not as effective and Kaylee's reflux started messing with her heart stuff. Just as we had started going to 3 hourly feeds rather than hourly or continuous - which was a big step toward "normal" - we had to place an NJ tube instead of her NG tube. This is a tube which goes through her stomach and sits in her small intestine. I love the NJ tube because without it Kaylee's heart condition would still be requiring her to be in hospital. I love the NJ tube because without it Kaylee (whose reflux has gotten more and more severe) would probably vomit a large portion of what she was fed and would not be growing or putting on weight at the rate that she needs to so she can get ready for her surgery. I love the NJ tube because it keeps my baby alive! It gets my milk into her which has helped her stay reasonably healthy and grow delightful fat rolls. It means I can give her medicine without worrying about her vomiting it up or spitting it out. I can keep her well hydrated - a very important thing as dehydration could make her shut stop working. But I hate it for every other reason.
The NJ tube needs to be placed by a radiologist so they can take pictures of where it is which means if it gets clogged or kinked we need to go to hospital - and if that happens after hours (which, for some reason, it almost always does) we need to stay overnight until they come in the next day.
The NJ tube means that Kaylee must be fed small amounts continually. This means she does not get hungry - which SOUNDS good. But learning what hunger means and that one needs to eat to stop feeling hungry is something that most babies do without us really thinking about it. Right now Kaylee is not learning that lesson. The cycle of hunger and feeding also means that a baby wakes up and interacts with either Mum or Dad and uses mouth muscles (the same muscles used for speaking, chewing, swallowing saliva etc. - all things that Kaylee was going to find challenging anyway with her other issues) several times a day - and in some cases several times a night! The nerves that feel the sensations of hunger, being touched and held for a feed, milk being drunk, tummies getting full all send messages to the brain not only about food and eating but about where the baby's body is in space (sitting, lying, being touched etc) and the brain creates pathways with this information which we use every day for our whole lives without even thinking about it. To help Kaylee develop these pathways I massage her gums, give her skin-to-skin contact, put expressed milk on her dummy so she can experience taste (she used to suck her dummy but since her reflux has worsened Kaylee has largely lost her sucking abilities, we will have to re-teach her to suck). There are fabulous therapists who will help us with all of these things as we come to them. So as with most big medical interventions, there is the good AND the bad.
After Kaylee's heart surgery we will start doing more with her feeding tube. Trying out an NG which is a tube through her nose to her stomach (which I can learn to place at home, eliminating the need for quite so many hospital visits). We may have a G tube placed which goes through her the wall of her tummy into her stomach and sometimes (in the case of a GJ) into her intestines which would eliminate the irritation of a tube in her nose and throat. Perhaps we will be able to move to bolus feeds where we give feeds every few hours rather than continuously which would be wonderful. There is no reason why Kaylee can't start to learn to eat "normally" as we get her other health issues sorted out - but it will take her a while. In the mean time I will be able get all the breastmilk and medicines into her which she needs.
We have learned just how common the tubie experience is since we were introduced to this world. It isn't just people who are as unwell as Miss K. There are some people who look "normal" who lift their shirts and hook up a pump to their belly for a feed. For most who have them a tube is a life improving - if not life giving - measure and the best chance they've got at getting well. We have been blessed by the knowledge, support and information provided by other tubie families and support groups and it helps us make informed choices for Miss Kaylee, our little tulip.
So that's how we got here and this is where we are going for now. If you ever find yourself in a position where you are having to manage a feeding tube there are some links to resources at the bottom of our Cornelia De Lange page

No comments:
Post a Comment